-
Reviewed
Key takeaways
- The vulva is the external part of the female genitals. The vagina is an internal tube that connects your vulva to the lower part of your uterus.
- Everyone’s vulva is unique in shape, size and colour.
- It’s important to take care of your vulva, and understand what’s normal for you.
- See your doctor if you notice any unusual changes.
Key takeaways
- The vulva is the external part of the female genitals. The vagina is an internal tube that connects your vulva to the lower part of your uterus.
- Everyone’s vulva is unique in shape, size and colour.
- It’s important to take care of your vulva, and understand what’s normal for you.
- See your doctor if you notice any unusual changes.
What is the difference between your vulva and vagina?
Some people think the vulva is the vagina, but they’re different.
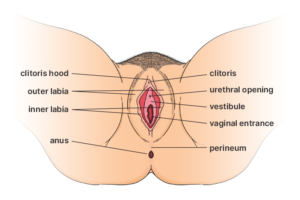
The vulva is the outside part of the female genitals that you can see. It includes:
- the clitoris and clitoris hood
- the outer lips (labia), which are covered with pubic hair
- the inner lips (labia)
- the urethral opening (where wee comes out)
- the area around your vaginal and urinary openings (vestibule)
- the vaginal entrance
- the area of skin between your vagina and anus (perineum).
Your vagina is a tube inside your body that connects your vulva to the lower part of your uterus (cervix). It’s where your period flows down from the uterus, where you can have vaginal sex and where babies pass through during childbirth.
Are all vulvas and vaginas the same?
Everyone’s vulva is unique in size, shape, colour and appearance. It’s normal for the left and right sides of your vulva to be different in shape and size, especially the inner lips (labia).
It’s a good idea to see what your vulva looks like. You can use a mirror to see what is normal for you. This will make it easier to notice any changes in appearance, for example, changes in colour or skin.
Try not to compare yourself to images you see online – many of these are edited. Instead, check out the Labia library for photos of real labia.
It’s normal for your vulva and vagina to have a different smell at certain times during your menstrual cycle, and after menopause.
There are many fluids associated with the vulva that can affect how it smells. For example:
- urine (wee)
- sweat
- menstrual blood
- skin oils
- vaginal and gland secretions.
If the smell is unpleasant, yeasty or fishy smelling, this may be a sign of an infection. An unpleasant smell may also be due to a sexually transmitted infection (STI), a tampon that needs to be changed, or not wiping thoroughly after going to the toilet.
After menopause, the smell may be different because the bacteria in your vagina changes.
If you’re worried about the smell or have other symptoms, see your doctor.
Hormonal changes after childbirth, while breastfeeding and around menopause can make the vulva and vagina feel dry.
You may have a loss of natural lubrication, which can cause painful sex.
A guide to vulval self-checks
Your vulva is the external part of the female genitals that you can see. No two vulvas look the same. It’s important to get to know the look and feel of your vulva. That way, you can spot changes more easily and tell your doctor.
- Use a mirror: Ensure you have good lighting. Stand with one leg up or squat over the mirror.
- While showering: Use your fingers to feel for changes.
- Check your undies: Look for unusual discharge, including a change in colour, smell or texture.
- With clean hands and using a mirror, look at and feel the areas covered with pubic hair.
- Gently part the outer skin folds and check the inner, hairless folds.
- Check the skin around your vagina and urinary opening (where wee comes out).
- Check the skin between your vagina and anus.
- If something doesn’t look or feel normal for you, visit your doctor.
Look and feel for changes in your vulva, like:
- a new lump
- a cut, rash or ulcer
- soreness or itchiness
- new or changing freckles or moles
- unusual discharge or unusual bleeding.
You can learn more about vulva self-checks in this Q&A with GP and sexual health expert Dr Sara Whitburn.
How to care for your vulva
There are many things you can do to look after your vulva and reduce the risk of vulval irritation.
Use soap-free products or just water to wash your vulva. Avoid using perfumed soaps and bath products, douches or vaginal washes as these may irritate your vulva.
Never use talcum powder on your vulva, as it can cause inflammation.
Wear natural fibre underwear, such as cotton, because:
- they’re breathable
- they’re less likely to cause an allergic reaction than synthetic fabrics, like polyester.
Wash your underwear in pure or unscented soap.
Avoid tight-fitting jeans and pants. And if you wear pantyhose, make sure they have a cotton gusset.
After exercise, change or shower straight away. Lycra and sweat can irritate your vulva.
If you swim in chlorinated water, you can use a barrier ointment to avoid vulval irritation. These ointments are available in most chemists and supermarkets.
After swimming, try to shower straight away. Wash your vulva to remove any chlorine or salt from the pool.
After you go to the toilet, wipe or pat your vulva from front to back. And try to use white, unscented toilet paper.
Use 100% cotton sanitary pads and tampons, and change them regularly.
If your menstrual blood irritates your vulva, you can use tampons or a menstrual cup instead of pads.
If you need extra lubrication when having vaginal sex, use silicone-based or water-based lubricants.
You can also use good-quality natural oils, such as olive or almond oil. Don’t use oil-based lubricants when using a condom, as the condom may break.
Vulval irritation and treatment
Vulval irritation is common and usually caused by sensitivities, infections, hormonal changes or skin conditions affecting the delicate skin of the vulva. This page explains common symptoms, possible causes, self-care and medical treatments, and when to see your doctor.
Vulval and vaginal conditions
Conditions affecting the vulva and vagina are common and often have similar symptoms, but most improve with the right diagnosis and treatment. This page explains common vulval and vaginal conditions, what symptoms to look out for, treatment options, and when to see your doctor.
Vulval and vaginal pain
Vulval and vaginal pain is common and can be caused by conditions like vulvodynia, vulval or vaginal tears, or pudendal neuralgia. Symptoms may include burning, stinging or pain with sex, tampons or sitting. If you have ongoing pain, it’s important to see your doctor for an examination and the right treatment.
Pelvic organ prolapse
Pelvic organ prolapse occurs when weakened pelvic floor muscles allow the bladder, bowel or uterus to drop down into the vagina. Symptoms can include vaginal heaviness, bulging and bladder or bowel problems. See your doctor early, as treatment like pelvic floor exercises or physiotherapy can help prevent it from getting worse.
Personal stories about vulval and vaginal health
Our review process
This information has been reviewed by clinical experts and is based on the latest evidence.
Our content review process ensures our health information is accurate, trustworthy, current and useful.
We regularly check our information to make sure it reflects the latest clinical guidelines and key findings from large, reliable studies.
Where possible, we focus on Australian research to make our information more relevant locally.
Experts play a key role in reviewing our content. Clinicians at Jean Hailes check information for accuracy and real‑world relevance. These include GPs, gynaecologists, endocrinologists, psychologists and allied health professionals.
We also work with partner organisations, independent specialists and people with lived experience to make sure our content reflects both expert knowledge and the experiences of the community.

Health information in your language
You might want to know more about

Sex and sexual health

Gynaecological cancers





















