-
Reviewed
Key takeaways
- Uterine cancer is the most common gynaecological cancer diagnosed in Australia.
- Symptoms can include unusual vaginal bleeding, pelvic pain and painful sex.
- Talk to your doctor if you notice any of these symptoms. They may not be due to cancer, but it’s important to check.
- As with many cancers, early detection leads to the best treatment outcomes.
Key takeaways
- Uterine cancer is the most common gynaecological cancer diagnosed in Australia.
- Symptoms can include unusual vaginal bleeding, pelvic pain and painful sex.
- Talk to your doctor if you notice any of these symptoms. They may not be due to cancer, but it’s important to check.
- As with many cancers, early detection leads to the best treatment outcomes.
What is uterine cancer?
Uterine cancer occurs when abnormal cells grow in the lining or muscle of the uterus. It’s the most diagnosed gynaecological cancer in Australia, mainly affecting women aged over 50.
There are 2 main types of uterine cancer:
- endometrial cancer – the cancer starts in the lining of the uterus
- uterine sarcoma – a rare cancer that develops in the muscle or tissues of the uterus.
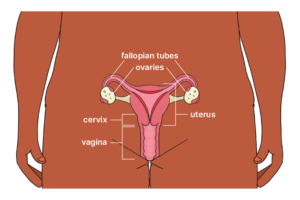
Symptoms of uterine cancer
The most common symptom of uterine cancer is unusual vaginal bleeding, particularly bleeding after menopause.
Other common symptoms include:
- periods that are heavier than usual, or a change to your periods
- bleeding in between periods
- periods that continue without a break.
Less common symptoms include:
- watery, smelly discharge
- unexplained weight loss
- discomfort or pain in your belly
- painful sex
- difficulty weeing.
Talk to your doctor if you are worried about any of these symptoms. They may not be due to cancer, but it’s important to check.
Causes of uterine cancer
The exact cause of uterine cancer is not known, but it may be associated with:
- a family history of cancer
- certain genetic conditions
- endometrial hyperplasia – a condition where the lining of the uterus is thicker than normal)
- other health factors.
How is uterine cancer diagnosed?
You can’t screen for uterine cancer, so it’s important to see your doctor if you notice any symptoms.
Your doctor will ask about your:
- symptoms
- medical history
- family medical history.
They may do a physical examination to check your:
- vulva, vagina and cervix
- uterus and pelvis.
They might also ask you to do blood and urine (wee) tests.
If your results suggest you may have uterine cancer, your doctor will refer you to a gynaecological oncologist (a specialist in gynaecological cancers) straight away.
You may need more tests to diagnose uterine cancer. For example:
- an internal ultrasound (via the vagina) to look at your ovaries and uterus
- a procedure to take a sample of cells from your uterus lining
- imaging tests – to check if cancer has spread outside your uterus.
Treatments for uterine cancer
Treatment for uterine cancer depends on the extent of the cancer. It may include:
- surgery
- radiotherapy
- hormone therapy (usually in advanced stages)
- chemotherapy
- palliative treatment.
Some cancer treatments, such as chemotherapy and radiotherapy, can cause menopause.
When to see your doctor about uterine cancer
It’s important to see your doctor if you notice any symptoms of uterine cancer. As with many cancers, early detection leads to the best treatment outcomes.
More resources on uterine cancer
For more information about uterine cancer, visit the:
If you would like to speak to a nurse for general information and support, call Cancer Council on 13 11 20 (9 am to 5 pm, Monday to Friday).
Personal stories about gynaecological cancers
Our review process
This information has been reviewed by clinical experts and is based on the latest evidence.
Our content review process ensures our health information is accurate, trustworthy, current and useful.
We regularly check our information to make sure it reflects the latest clinical guidelines and key findings from large, reliable studies.
Where possible, we focus on Australian research to make our information more relevant locally.
Experts play a key role in reviewing our content. Clinicians at Jean Hailes check information for accuracy and real‑world relevance. These include GPs, gynaecologists, endocrinologists, psychologists and allied health professionals.
We also work with partner organisations, independent specialists and people with lived experience to make sure our content reflects both expert knowledge and the experiences of the community.















