-
Reviewed
Key takeaways
- The ovaries produce, store and release eggs. They also produce hormones that control your periods.
- The uterus is part of the female reproductive system. It’s where babies grow during pregnancy.
- Many conditions affect these parts of your body.
- See a doctor if you have pain in the pelvis or belly (abdomen), unusual bleeding or discharge from the vagina, or pain when weeing.
Key takeaways
- The ovaries produce, store and release eggs. They also produce hormones that control your periods.
- The uterus is part of the female reproductive system. It’s where babies grow during pregnancy.
- Many conditions affect these parts of your body.
- See a doctor if you have pain in the pelvis or belly (abdomen), unusual bleeding or discharge from the vagina, or pain when weeing.
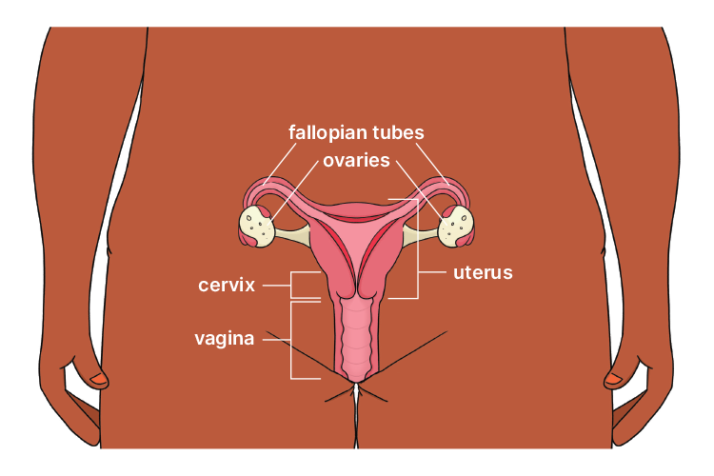
What are ovaries?
Ovaries are small oval-shaped organs that produce, store and release eggs (ovulation). They also make female hormones that control your menstrual cycle, periods and pregnancy.
Women are usually born with 2 ovaries, one on each side of the uterus.
What is a uterus?
The uterus (womb) is a muscular organ that sits in the belly (abdomen).
The lower part of the uterus connects to the vagina. The uterus is part of the female reproductive system. It’s where period blood come from and where babies grow.
Adenomyosis
Adenomyosis is a condition where tissue similar to the lining of the uterus grows into the muscle wall, often causing painful and heavy periods and pelvic pain. This page explains the symptoms, possible causes, how adenomyosis is diagnosed, and the treatment options available, including hormone medicines and surgery.
Fibroids
Fibroids are common, noncancerous growths in the muscle wall of the uterus that can cause symptoms such as heavy or painful periods and irregular bleeding, though many people have no symptoms at all. This page explains what fibroids are, how they’re diagnosed, treatment options, and when to see your doctor.
Hysterectomy
A hysterectomy is surgery to remove the uterus and may be recommended for conditions such as fibroids, endometriosis or cancer. This page explains the different types of hysterectomy, why it may be needed, how it’s performed, and the benefits and risks to help you make an informed decision with your doctor.
Cervical and uterine polyps
Learn about cervical and uterine polyps, including their symptoms, causes, treatments and when to see a doctor.
Ovarian cysts
Learn about ovarian cysts, including their symptoms, causes, treatments and when to see a doctor.
Endometrial hyperplasia
Endometrial hyperplasia is a condition where the lining of the uterus becomes abnormally thick, often causing heavy or irregular bleeding. This page explains the symptoms, causes, risk factors, how it’s diagnosed, and treatment options, including hormone therapy and surgery.
Our review process
This information has been reviewed by clinical experts and is based on the latest evidence.
Our content review process ensures our health information is accurate, trustworthy, current and useful.
We regularly check our information to make sure it reflects the latest clinical guidelines and key findings from large, reliable studies.
Where possible, we focus on Australian research to make our information more relevant locally.
Experts play a key role in reviewing our content. Clinicians at Jean Hailes check information for accuracy and real‑world relevance. These include GPs, gynaecologists, endocrinologists, psychologists and allied health professionals.
We also work with partner organisations, independent specialists and people with lived experience to make sure our content reflects both expert knowledge and the experiences of the community.


















