-
Reviewed
Key takeaways
- Urinary incontinence (accidental wee leakage) is a common condition.
- Wee leakage isn’t normal and can be treated.
- Your doctor can help find the cause and recommend treatment options.
Key takeaways
- Urinary incontinence (accidental wee leakage) is a common condition.
- Wee leakage isn’t normal and can be treated.
- Your doctor can help find the cause and recommend treatment options.
What is urinary incontinence?
Urinary incontinence is when you have accidental wee leakage. It’s a common condition that can be treated, managed and sometimes cured.
How does a normal bladder work?
A normal bladder:
- can hold up to 600 ml of wee
- empties 4 to 6 times each day (every 3 to 4 hours) and up to once each night
- empties completely when you wee
- gives you enough time to get to the toilet
- doesn’t leak wee.
Types of urinary incontinence
There are different types of urinary incontinence, including:
- urge incontinence – you have a strong urgency to wee and can’t hold on long enough to get to the toilet, or you wee a lot during the night
- stress incontinence – wee leaks when you sneeze, cough, laugh or jump
- mixed incontinence – you experience urge and stress incontinence symptoms
- overflow incontinence – the bladder doesn’t empty properly and becomes overfull, causing it to leak.
What causes urinary incontinence?
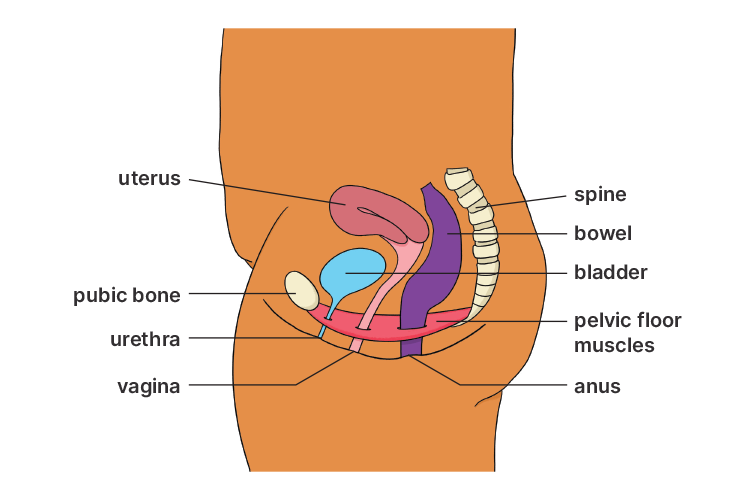
The pelvic floor muscles (muscles that support the bladder, bowel and uterus) can stretch and weaken, leading to incontinence.
Incontinence can also happen when pelvic floor muscles are too tight (overactive).
Some causes of urinary incontinence are:
- pregnancy and childbirth
- pelvic organ prolapse
- constipation or pushing hard when doing a poo
- repetitive lifting of heavy weights – at the gym, at work, in the garden or even when lifting children
- being overweight or obese
- coughing caused by smoking and chronic lung disease
- chronic sneezing (e.g. due to hay fever).
Urinary incontinence is also associated with:
- changes around the time of menopause (the pelvic floor becomes weaker and the bladder less elastic)
- diabetes
- pelvic or abdominal surgery
- certain medicines, such as fluid tablets (diuretics).
How to get a diagnosis
If you have symptoms of urinary incontinence, talk to your doctor or a continence nurse specialist.
They will ask about your medical history and symptoms, including:
- how often you go to the toilet
- how often you have wee leakage
- how much wee leaks
- when the wee leaks
- whether there is a burning sensation when you wee
- whether your bladder feels empty after weeing
- how often you wee during the day and at night
- how much fluid you drink.
They may test a urine sample for a urinary tract infection (UTI) or refer you to a specialist to do a pelvic floor muscle assessment.
Prevention and management of urinary incontinence
There are many ways to prevent and manage urinary incontinence. For example:
- eat a balanced diet
- do regular physical activity and maintain a healthy weight
- do regular pelvic floor muscle exercises
- practise good toilet habits, such as only weeing when you need to, not ‘just in case’
- talk to your doctor about hormone medicines that might help.
Learn more about managing urinary incontinence by visiting the Continence Health Australia website.
Our review process
This information has been reviewed by clinical experts and is based on the latest evidence.
Our content review process ensures our health information is accurate, trustworthy, current and useful.
We regularly check our information to make sure it reflects the latest clinical guidelines and key findings from large, reliable studies.
Where possible, we focus on Australian research to make our information more relevant locally.
Experts play a key role in reviewing our content. Clinicians at Jean Hailes check information for accuracy and real‑world relevance. These include GPs, gynaecologists, endocrinologists, psychologists and allied health professionals.
We also work with partner organisations, independent specialists and people with lived experience to make sure our content reflects both expert knowledge and the experiences of the community.

Want to learn more about pelvic floor exercises?
Join pelvic floor physiotherapist Janetta Webb on our podcast for simple exercises that strengthen your pelvic floor.