- What is cervical cancer?
- Can you screen for cervical cancer?
- HPV vaccine
- Symptoms of cervical cancer
- Causes of cervical cancer
- Can you reduce your risk for cervical cancer?
- How is cervical cancer diagnosed?
- Treatments for cervical cancer
- When to see your doctor about cervical screening
- More resources on cervical cancer
-
Reviewed
Key takeaways
- Cervical cancer is usually caused by the human papillomavirus (HPV).
- Regular cervical screening prevents 9 out of 10 cervical cancers, so it’s important to keep your health checks up to date.
- Early symptoms of cervical cancer include unusual vaginal bleeding, painful sex and pelvic pain.
- Talk to your doctor if you notice any of these symptoms. They may not be due to cancer, but it’s important to check.
- As with many cancers, early detection leads to the best treatment outcomes.
Sections on this page
- What is cervical cancer?
- Can you screen for cervical cancer?
- HPV vaccine
- Symptoms of cervical cancer
- Causes of cervical cancer
- Can you reduce your risk for cervical cancer?
- How is cervical cancer diagnosed?
- Treatments for cervical cancer
- When to see your doctor about cervical screening
- More resources on cervical cancer
Key takeaways
- Cervical cancer is usually caused by the human papillomavirus (HPV).
- Regular cervical screening prevents 9 out of 10 cervical cancers, so it’s important to keep your health checks up to date.
- Early symptoms of cervical cancer include unusual vaginal bleeding, painful sex and pelvic pain.
- Talk to your doctor if you notice any of these symptoms. They may not be due to cancer, but it’s important to check.
- As with many cancers, early detection leads to the best treatment outcomes.
What is cervical cancer?
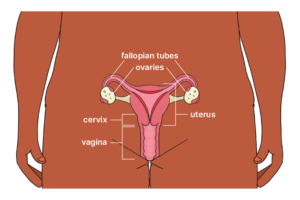
Cervical cancer develops in the cervix (the entrance to the uterus). This cancer is usually caused by the human papillomavirus (HPV).
Cervical cancer can start in the squamous or glandular cells. Some cervical cancers have both squamous and glandular cells. Cancer in the squamous cells is the most common type of cervical cancer.
Cervical cancer can occur at any age, but it’s more common in people aged over 30.
Can you screen for cervical cancer?
Yes, you can. It’s important to have regular cervical screening tests to check for the human papillomavirus (HPV). Regular screening prevents 9 out of 10 cervical cancers.
HPV vaccine
HPV is a common sexually transmitted infection (STI) that can affect the surface of the cervix, vagina and vulva.
The best time to get immunised against HPV is before you become sexually active. Under the National Immunisation Program, people aged 12 to 13 get a free HPV vaccine at school.
If you have been vaccinated for HPV, it’s still important to get regular cervical screening tests. While the HPV vaccine is highly effective, it doesn’t prevent all HPV infections.
For more information about the HPV vaccine, see your doctor or visit the Australian Government Department of Health and Aged Care website.
Symptoms of cervical cancer
You might not have any symptoms of cervical cancer, especially in the early stages. But symptoms can include:
- periods that are longer or heavier than usual
- bleeding between periods
- bleeding after sex
- bleeding after menopause
- painful sex
- unusual vaginal discharge
- pelvic pain.
Symptoms of advanced cervical cancer include:
- feeling very tired
- leg pain or swelling
- lower back pain.
Talk to your doctor if you notice any of these symptoms. They may not be due to cancer, but it’s important to check.
Causes of cervical cancer
Cervical cancer is almost always caused by the human papillomavirus (HPV). HPV is a common sexually transmitted infection (STI) that can affect the surface of the cervix, vagina and vulva.
About 80% of women will have the virus at some point in their lives, but many don’t know they’ve been exposed to the infection.
Most women with the infection don’t develop cervical cancer. Only certain types of HPV cause cancer.
Cervical cancer usually develops many years after the HPV infection occurs.
Can you reduce your risk for cervical cancer?
You can reduce your risk for cervical cancer by:
- not smoking
- having regular cervical screening tests
- having the HPV vaccine.
How is cervical cancer diagnosed?
A cervical screening test will check for the human papillomavirus (HPV). If HPV is not detected, you can wait 5 years until your next test.
If your results suggest you may have cervical cancer, your doctor will refer you to a gynaecological oncologist straight away.
If you have an abnormal test result, you may need further tests or procedures. For example, a second cervical screening test or a colposcopy.
Treatments for cervical cancer
If precancerous cells are detected, your doctor may recommend:
- laser therapy – to remove abnormal cells and tissue (performed under local anaesthetic)
- a loop excision – to remove abnormal cells from the surface of the cervix (performed under local or general anaesthetic)
- a cone biopsy – to remove a larger area of the cervix (performed under general anaesthetic).
Treatment for cervical cancer depends on the extent of the cancer. It may include:
- surgery
- radiotherapy
- chemotherapy
- palliative treatment.
Some cancer treatments, such as chemotherapy and radiotherapy, can cause menopause.
When to see your doctor about cervical screening
See your doctor for regular cervical screening tests. You can also ask your doctor about the HPV vaccine if you haven’t already had it.
It’s important to see your doctor if you notice any symptoms of cervical cancer. As with many cancers, early detection leads to the best treatment outcomes.
More resources on cervical cancer
For more information about cervical cancer, visit the:
- Cancer Australia website
- National Cervical Screening Program website
- Australian Cervical Cancer Foundation website
For more information about cervical screening and the HPV vaccine, visit the Cancer Council cervical screening webpage.
If you would like to speak to a nurse for general information and support, call Cancer Council on 13 11 20 (9 am to 5 pm, Monday to Friday).
Our review process
This information has been reviewed by clinical experts and is based on the latest evidence.
Our content review process ensures our health information is accurate, trustworthy, current and useful.
We regularly check our information to make sure it reflects the latest clinical guidelines and key findings from large, reliable studies.
Where possible, we focus on Australian research to make our information more relevant locally.
Experts play a key role in reviewing our content. Clinicians at Jean Hailes check information for accuracy and real‑world relevance. These include GPs, gynaecologists, endocrinologists, psychologists and allied health professionals.
We also work with partner organisations, independent specialists and people with lived experience to make sure our content reflects both expert knowledge and the experiences of the community.
