-
Reviewed
Key takeaways
- Many women experience breast tenderness, discomfort or pain at different times.
- Common breast conditions include painful breasts, lumps and cysts.
- See your doctor if you are concerned about changes in your breasts or nipples.
Key takeaways
- Many women experience breast tenderness, discomfort or pain at different times.
- Common breast conditions include painful breasts, lumps and cysts.
- See your doctor if you are concerned about changes in your breasts or nipples.
What are breasts?
Females and males have breasts, but they are different in size, shape and function.
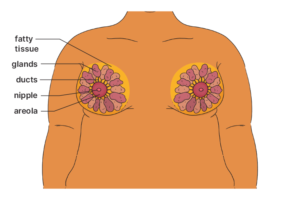
The inside of your breasts
Your breasts have 15 to 20 lobes with glands that produce milk and ducts that take milk to the nipple.
Fatty and fibrous tissue surrounds the lobes, giving breasts their size and shape.
Breasts also have blood vessels, lymph glands and nerves.
The outside of your breasts
The nipple is the small bump in the middle of each breast. This is where milk comes out to feed a baby. Around the nipple is a darker circle of skin called the areola.
What’s normal?
It’s normal for:
- one breast to be bigger than the other
- breasts to feel lumpy.
Normal changes in your breasts
It’s normal for breast tissue to change throughout your life. These changes can happen:
- during your menstrual cycle
- during pregnancy
- while breastfeeding
- as you age.
Every menstrual cycle, the hormones in your body change. This can make your breasts:
- feel sore or tender
- feel more lumpy than usual
- look a bit different.
You may notice these changes just before your period starts.
If you are pregnant or breastfeeding, you’ll notice that your breasts change as they get ready to make milk for the baby.
As you approach menopause (your final period), oestrogen hormone levels drop, which may cause breast discomfort.
After menopause, breasts may feel softer.
How breast density affects screening and cancer risk
Breast density describes the appearance of breast tissue on a breast mammogram (X-ray). Dense breasts are quite common. Research suggests about 23% of women in Australia have dense breasts.
A mammogram shows the ratio of dense tissue to fatty tissue in your breasts. Dense tissue shows up as white on a mammogram, while fatty tissue appears dark.
Dense breasts make cancer detection harder because cancer also appears white on mammograms, making tumours harder to spot.
Increased breast density is associated with an increased risk of breast cancer.
Currently, women in New South Wales, South Australia, Western Australia and Victoria receive breast density information as part of their routine screening. Other states in Australia are working towards including it in screening.
If your mammogram shows dense breasts, it’s important to talk to your doctor. They might recommend additional tests, such as ultrasound or an MRI.
Read more about breast density and screening on the Breast Cancer Network Australia website.
Common breast conditions
Many conditions can affect your breasts. Learn more about the conditions, symptoms and treatments.
Many women experience breast pain, but the cause isn’t known. In younger women, it’s often linked to the menstrual cycle. You may also have breast pain around the time of menopause.
The Pill and menopausal hormone therapy (MHT) can also cause breast discomfort in some women.
You may be able to relieve breast tenderness or pain by:
- applying cool packs or heat packs to the affected area
- taking a warm shower or bath
- wearing a comfortable, supportive bra – or no bra
- trying different relaxation techniques
- taking pain-relief medicine.
To help with breast pain, your doctor may suggest you take 1,000 mg of evening primrose oil up to 3 times a day (with food) for a few months.
Painful breasts are not normally a symptom of breast cancer, but if the pain doesn’t go away, see your doctor.
Normal breast tissue is lumpy. You may notice lumps in the upper area of the breast. It’s normal for your breasts to feel lumpy before your period and less lumpy after your period.
Fibroadenomas are painless, benign breast lumps made up of glands and fibrous tissue. These lumps feel quite smooth and firm and can be moved within the breast tissue.
Fibroadenomas are more common in women between the ages of 15 and 30. But they can occur in older women. A recent study showed that 10% of women have fibroadenoma at least once in their lifetime.
Most lumps are small, but they can grow to as large as a golf ball. They can also be tender in the days before your period.
A breast cyst is a fluid-filled sac in the breast tissue. Cysts can vary in size during your menstrual cycle and may disappear on their own.
Breast cysts are harmless, but they can be painful. They commonly occur in women aged 35 to 50, but they can also occur in younger women.
Some women have a combination of cysts and thickened breast tissue. This is called ‘benign fibrocystic disease’. It can cause lumpy breasts, and pain and tenderness that fluctuates during your menstrual cycle.
The risk of benign fibrocystic disease increases with age. It usually disappears after menopause but may persist if you take MHT.
Any fluid leaking from your nipples is referred to as nipple discharge.
When you’re pregnant or breastfeeding, it’s normal for discharge or milk to leak from your nipples. This eventually stops after you stop breastfeeding.
Depending on the cause, discharge may be
- milky
- clear
- yellow
- green
- brown
- bloody.
The consistency can be thick and sticky or thin and watery.
Discharge may be caused by hormone changes, duct problems, trauma or infection. But it can also be a sign of breast cancer. It’s important to see your doctor if you notice:
- discharge that is watery or blood-stained
- discharge and a lump
- a change in your nipple (e.g. a ‘tucked in’ or inverted nipple).
With mastitis, you might notice changes in the breast tissue, such as:
- redness
- heat
- lumpiness
- pain.
You can also experience flu-like symptoms, such as fever and chills.
Mastitis most commonly occurs in women who are breastfeeding because blocked milk ducts get infected.
Treatment may include:
- antibiotics for the bacterial infection
- anti-inflammatory medicine to relieve inflammation and pain
- continuing to breastfeed or express milk, as draining the breast helps clear the blocked ducts.
You need to start antibiotics right away to prevent pus from building up and forming an abscess. If an abscess develops, you may need to a small surgical procedure to drain it.
Mastitis can also happen if you aren’t breastfeeding. In these cases, it’s important to see your doctor.
It’s common to have itchy nipples or breasts. Itchiness can be caused by:
- skin disorders, such as eczema or psoriasis
- skin infection, such as thrush (fungal) or mastitis (bacterial)
- contact dermatitis (e.g. from soap or clothing)
- dry skin
- hormonal changes.
Nipple and breast itchiness is not normally a symptom of breast cancer, but it can be. If you have concerns, it’s important to see your doctor.
Breast cancer
Breast cancer is cancer that starts in the cells of the breast and may cause changes such as a lump, nipple discharge, or changes in breast appearance. This page explains breast cancer risk factors, the importance of being breast aware, and screening with mammograms to help detect cancer early.
Personal stories about breast cancer
Our review process
This information has been reviewed by clinical experts and is based on the latest evidence.
Our content review process ensures our health information is accurate, trustworthy, current and useful.
We regularly check our information to make sure it reflects the latest clinical guidelines and key findings from large, reliable studies.
Where possible, we focus on Australian research to make our information more relevant locally.
Experts play a key role in reviewing our content. Clinicians at Jean Hailes check information for accuracy and real‑world relevance. These include GPs, gynaecologists, endocrinologists, psychologists and allied health professionals.
We also work with partner organisations, independent specialists and people with lived experience to make sure our content reflects both expert knowledge and the experiences of the community.

