There are two main types of uterine cancer: endometrial cancer and uterine sarcoma. Endometrial cancer is the most diagnosed gynaecological cancer. Uterine sarcoma is a much rarer cancer. Learn more about these cancers, the symptoms, causes and how they are diagnosed.
Cancer of the uterus – endometrial cancer
Cancer of the uterus – uterine sarcoma
Symptoms
Causes
Diagnosis
Treatment
When to see your doctor
Related resources
Endometrial cancer occurs in the lining of the uterus. It is the most diagnosed gynaecological cancer, mostly in people over the aged over 50 who have a uterus. It’s also the most common uterine cancer.
The below picture shows the female reproductive organs.
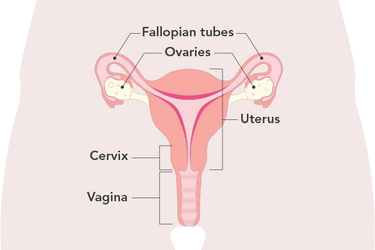
Uterine sarcoma is a rare uterine cancer that forms in either the muscle of the uterus or the cells in the lining of the uterus. It occurs in about 2% to 5% of all uterine tumours and less than 1% of all gynaecological cancers. It’s more likely to occur after menopause.
Symptoms and diagnosis of uterine sarcoma are similar to those of endometrial cancer.
If the uterine sarcoma is confined to the uterus, it is usually treated with surgery.
The most common symptom of uterine cancer (including endometrial cancer and uterine sarcoma) is unusual bleeding, particularly bleeding after menopause.
Other common symptoms may include:
Less common symptoms may include:
See your doctor if you have any of these symptoms. They may be due to other conditions, but it’s important to check.
We don’t know the exact cause of uterine cancer, but it may be associated with:
Some women who develop uterine cancer don’t have any risk factors. But risk factors can include:
Like many cancers, early diagnosis and detection lead to the best treatment outcomes.
As there is no known way to screen for uterine cancer, it’s important to see your doctor if you notice any symptoms.
Uterine cancer is usually diagnosed via a clinical examination. Your doctor will ask about your symptoms, medical history and family health history.
They may do some physical examinations to check your:
You may also need to have blood and urine (wee) tests.
If your examination and test results suggest you may have uterine cancer, your doctor will refer you to a gynaecological oncologist (a specialist in gynaecological cancers) straight away.
You may need more tests to diagnose uterine cancer. For example:
Treatment for uterine cancer depends on the extent of the cancer. It may include:
Cancer treatment, such as chemotherapy and radiotherapy, can cause menopause. Learn more about menopause due to cancer treatment.
It’s important to see your doctor if you notice any symptoms of uterine cancer. In most cases, early detection and diagnosis lead to good outcomes.
This web page is designed to be informative and educational. It is not intended to provide specific medical advice or replace advice from your health practitioner. The information above is based on current medical knowledge, evidence and practice as at April 2023.
This content has been reviewed by a group of medical subject matter experts, in accordance with Jean Hailes policy.
© Jean Hailes Foundation. All rights reserved. This publication may not be reproduced in whole or in part by any means without written permission of the copyright owner. Contact: licensing@jeanhailes.org.au